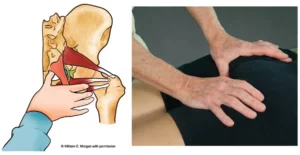
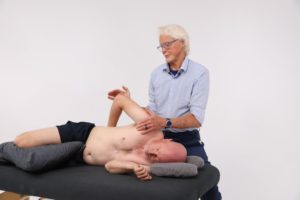
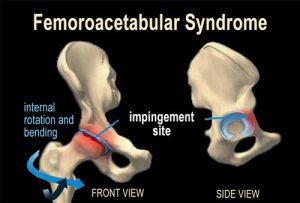
Most of the human race suffers some form of neck and back pain during their lifetime just as common as a headache, stomach ache or knee pain. “Until it was turned into a medical condition in the early 20th century, back pain was considered an inevitable human experience,” said Canadian surgeon Hamilton Hall, MD. “There is no simple cure because there is usually not a clear-cut precipitating trigger associated with many forms of musculoskeletal pain,” notes Hall.
Despite the liberal use of the words “back injury” across modern societies, most episodes of back pain do not have an obvious cause. “Research indicates that approximately two of every three people who experience pain in the spine are unable to identify any specific event that may have caused their problems,” states Hall. Back pain simply happens!
The modern perspective that neck and back pain is a variable, intermittent illness rather than a one-time condition should not be considered a threatening event for our clients. In the vast majority of cases, recurrences of these painful conditions are not signs of advancing disease, an omen of chronic disability or even a cause for significant worry.
Some researchers draw an analogy between back pain and upper respiratory infections. Many individuals get colds or respiratory infections several times each year, yet are typically not viewed as a significant threat to their health. Colds don’t require high-tech diagnostic testing, heroic treatment interventions or significant absence from work. These conditions, like most cases of neck/back pain, simply are bumps in the road.
However, some have begun to question the possibility of previously unrecognized neurobiological processes that might unravel the question: Why are some people more susceptible to pain than others? One interesting new area of pain management research that is gaining a great deal of attention proposes alternative ways that nerve impulses are transmitted and learned by the central nervous system.
Sensitization of Back Pain
For decades, it was thought that spinal cord, brain and peripheral pain transmission pathways were hardwired circuits whose job was simply to communicate pain signals from injured or diseased parts of the body to specific message centers in the brain. But based on recent scientific research, new ideas are emerging on how pain transmission actually works and how the brain has the ability to create the conscious experience of pain.
A process called sensitization has become a topic of great interest to neuroscientists studying transmission mechanisms of painful stimuli. The puzzling question is: How are pain messages actually delivered? A discussion of sensitization might help somatic practitioners better understand why a client’s chronic pain can be so severe, but in some cases, seem out of proportion to the degree of injury or disease in the affected body tissues. This understanding also might help explain why specific treatments directed at pain relief often provide only limited benefit.
The neurobiology of sensitization is extremely complex, but the basic idea behind it is fairly straightforward. When pain signals are transmitted from injured or diseased tissues, these signals can then activate (sensitize) pain circuits in the peripheral nervous system, spinal cord and brain by burning a memory pathway.
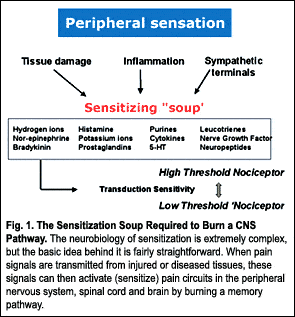
The process of sensitization can be compared to overly adjusting the volume control on a stereo system, thereby amplifying and sometimes distorting the pain message. This results in a painful condition that is severe and out of proportion to the actual dysfunction or original injury. Sensitization has the innate ability to alter all regions of the central nervous system that process pain messages. This includes the sensing, feeling and thinking centers of the brain. Here lies one explanation why chronic pain often is associated with, not only physical disorders, but also emotional and psychological suffering as well.
Phantom Limb Pain
A perfect example of the workings of sensitization can be found in the sometimes mysterious condition called phantom limb pain. In the presence of phantom limb pain, the client might feel intense pain in an area where the body part is missing. Common examples are seen in amputated arms and legs, as well as in women experiencing abdominal pain years after undergoing a hysterectomy. The difficult-to-treat problem of phantom limb pain is consciously actualized by persistent activation (sensitization) of the pain transmission pathways from the site of amputation up to the brain.
But what about the presence of sensitization in various pain conditions where amputation or surgeries to remove diseased organs don’t exist? Too often, manual therapy treatments in such cases are directed to body areas that were once actual pain-generators, (i.e., where the injured or diseased tissues once existed). Regrettably, “chasing the pain” by directing therapy to where the client currently is hurting will have little effect on the sensitized pain pathways in the spinal cord and brain. As a result, little benefit is experienced.
Having said that, the author has found that application of specific deep tissue and assisted stretching techniques to torsioned and compressed joint-related soft tissues co-activates and desensitizes noxious mechanoreceptive activity leading to a reduction in pain. Successful outcomes require the therapist concentrate treatment to areas proximal to the previously injured or amputated tissues (usually beginning in the lamina groove). Proper treatment to deep intrinsic muscles, spinal ligaments, joint capsules, and visceral structures co-activates a wider range of neuro-receptors, which enhances the desensitization process.
References
- Hall H. Consultation with a Back Doctor, McCleland & Stewart; 2003.
- Dalton E. Advanced Myoskeletal Techniques, pg. 72, Freedom From Pain Institute, 2005.
On sale this week only!
Save 25% off the "Dalton Technique Treasures" eCourse
The “Dalton Technique Treasures” eLearning course is a compilation of some of Erik’s favorite Myoskeletal Alignment Techniques (MAT). Learn MAT techniques to assess and address specific sports injuries, structural misalignment, nervous system overload, and overuse conditions. ON SALE UNTIL April 29th! Get Lifetime Access: As in all our eLearning courses, you get easy access to the course online and there is no expiry date.