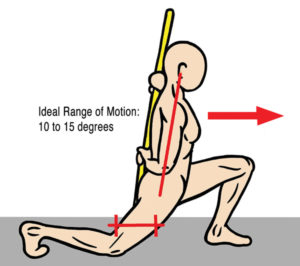
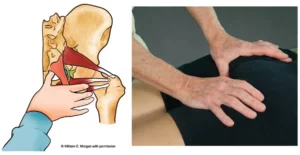
For decades, manual therapists, biomedical researchers and neuroscientists have battled over the conceptual ideology of pinched nerves. One group holds the belief that spinal misalignments cause or contribute to disease by choking “nerve energy” to body tissues. Others generally agree that the human body probably does possess some sort of universal energy system, but quickly point out that nerves do not appear as conductors of this “life-force” energy. To allow the reader to grasp both sides of this very important issue, this article will provide an overview of current theories that spur the controversy. Following an initial review of the various nerve impingement theories, let us review the two most pressing, yet basic, questions:
1. How do nerves get pinched?
2. Are pinched nerves really a contributing factor in common pain conditions observed daily in our offices and clinics?
One age-old premise supporting the pinched nerve theory follows this logic: If a spinal segment is not in its normal position, nerve pathways between the vertebrae (intravertebral foramina) will partially close resulting in nerve impingement. As the nerve root undergoes compression, soft tissues and organs supplied by the pinched nerve suffer from decreased nerve energy flow to the affected body parts. Thus, according to this theory, alterations in joint structure and function result not only in pain but an increased susceptibility to disease from spinal obstructions impinging on these nerves.
Detractors counter that nerves do not emit a flow of energy. Since nerves are gland cells, their primary function is to produce and release a hormone that causes muscle cell inhibition or contraction. Basically, that is all they do – no more, no less; therefore, these supporters believe that nerves do not actually conduct electricity or any other form of energy.
When a nerve cell undergoes its function of hormonal secretion, changes occur in its outer cell membrane allowing electrically charged ions to move in and out of the cell in a step-by-step fashion along the full extent of the nerve. This is often referred to as “conducting an impulse” or “firing.” A spinal nerve as it exits the intervertebral foraminal opening is actually a thin tube of connective tissue containing extensions of millions of nerve cells. These extensions are axons or “fibers.” The latter term appears misleading for it connotes a certain firmness similar to fine electrical wires. Sadly, nothing could be further from the truth.
Axons are delicate, flimsy structures. Since they consist of elongated or drawn out parts of cells, nourishment is needed along with the cells that make up their sheaths. Vital nutrients are supplied by blood vessels embedded in what is termed a “visible-level nerve.” If acute nerve compression does not directly kill the axons, they may die from compressive forces blocking blood flow within the vessels of the nerve. Nerve occlusion prevents axoplasmic flow of nutrients to be properly transported up and down the length of the nerve.
Another Snapshot of Pinched Nerves
The nerve root itself has been dismissed by most researchers as a pain-sensitive structure, although most clinicians do agree that nerve compression from herniated discs, spinal stenosis and spondylolisthesis can cause radiculopathies such as sciatica. Acute compression of a normal healthy nerve may lead to paresthesias, motor loss, sensory deficits and reflex abnormalities, but pain is absent. However, if an inflamed nerve suffering intraneural edema is compressed, pain is present. This “silent nerve root compression syndrome” hypothesizes that time is required for functional alterations, such as nerve tethering, to cause mechanical nerve fiber deformation and resulting pain.
Compression of an inflamed nerve anywhere along its extent can cause it to secrete its specific hormone. Pressure on an inflamed sensory nerve cell can cause the brain to experience pain (nociception). If an obstruction compresses a motor nerve cell, the hormone secretion can cause a muscle cell to contract (protective muscle spasm). When motor nerve cells to a skeletal muscle die from complete occlusion, the muscle becomes paralyzed as observed in extreme cases of sciatica and thoracic outlet syndrome. One of the first signs of complete nerve occlusion is muscle atrophy followed by a loss of normal neurological reflexes.
Nociceptive… or Pinched Nerve Pain?
Over the past decade, researchers working with magnetic resonance imaging (MRIs) have demonstrated that no matter how much a normally functioning spine is compressed or twisted, there is ample room in the intervertebral foramina for free movement of the nerve. It is postulated that in a healthy spine, nerve root compression shouldn’t exist even with all the intervertebral discs removed. Still, another viewpoint bears consideration.
Sprained capsules and ligaments cause joint mechanoreceptor hyperexcitability and protective muscle guarding. Muscles aren’t designed to be restraining tissues even though the deepest transversospinalis muscles are often awarded that task. As deep intrinsic muscles are subjected to abnormal sustained loading, nociceptive stimuli warn the brain of the possibility of tissue damage.
When nociceptors fire in response to actual tissue damage from macro- or microtrauma during routine daily activities, they quickly become major myofascial and spinal pain generators. Through a process called sensitization, an aberrant hard-wiring pattern is “burned” into the central nervous system (CNS). Long-term CNS agitation from angry nociceptors causes the brain to twist and torque the body in an effort to avoid pain.
Understanding and Treating the Dysfunction
As discussed earlier, the joint receptor concepts attempt to override the idea that pain is primarily a consequence of “pinched nerves” that could ultimately be freed by removing the bony or muscular obstruction. Many neurophysiologists now believe that restoration of proper postural alignment and range of motion successfully reduces pain by stimulating mechanoreceptors in fibrous joint capsules, spinal ligaments and transversospinalis muscles. To achieve a noticeable reduction of increased excitability in the neuronal pool, the pain-generating stimulus must be interrupted until the memory burned into the nerve cells has been completely “forgotten.” For many chronic pain cases, a “serial-type” deep tissue therapy works best where clients are seen twice weekly until hyperexcited receptors feeding the CNS are quieted.
Conclusion
Although spinal nerves travel through small intervertebral foramen openings, rarely does a bone-on-nerve dysfunction occur. Significant facet hypertrophy, disc collapse or intraneural edema must accompany the vertebral misalignment before the client experiences pain. While commonly associated with the spine, pinched nerve compressive lesions are actually rare.
What has made the “pinched nerve theory” so popular is that therapists viewing anatomy texts or cadavers can easily visualize how spinal nerves could become entrapped as they make their way through the bony little holes between vertebrae. Regrettably, nociceptors and mechanoreceptors cannot be seen.
For most of mankind, it is far easier to believe something we can see versus something invisible to the naked eye. Despite this human tendency, massage therapists must understand that spinal joints and muscles have massive nociceptive innervation that is profoundly affected by sustained compressional loading from tension, trauma and poor posture. While not clearly apparent, sensory receptors are the primary reason for client visits.
Click here for more information.
Special Savings this week only!
Save 25% off the "Myoskeletal Mobilization Massage Course"

NEW! Enhanced video USB format
Join Erik Dalton as he takes you on a step-by-step journey teaching you an efficient and effective method for assessing and correcting flexibility mobility issues we see every day in our practices. You will learn a full body routine that involves prone, sidelying, supine, and bench work. Follow along as Erik demonstrates how to use this as a stand alone routine or easily integrate the individual techniques into your massage practice.
Sale ends Monday May 6th. Click the button below for more information and to purchase the course for CE hours and a certificate of completion to display in your office. Bonus: Purchase the home study course and receive the eLearning course for FREE!