Any time an internal body part pushes into an area where it doesn’t belong, it’s called a hernia. When we eat, food travels down the esophagus passing though a small opening (hiatus) in the diaphragm, before entering the stomach. Normally, there are several mechanisms to prevent acid from flowing backwards (refluxing) up into the esophagus. The lower esophageal sphincter (LES) is a muscular valve located at the top of the stomach that opens to let food enter, and then closes to keep the digestive acids and food in the stomach. When the opening in the diaphragm weakens, it may not be able to hold the stomach and LES down and a piece of the stomach protrudes through the hiatus. A hiatal hernia occurs when the top of the stomach either rolls, or slides up into this opening and becomes stuck there (Image 1.).
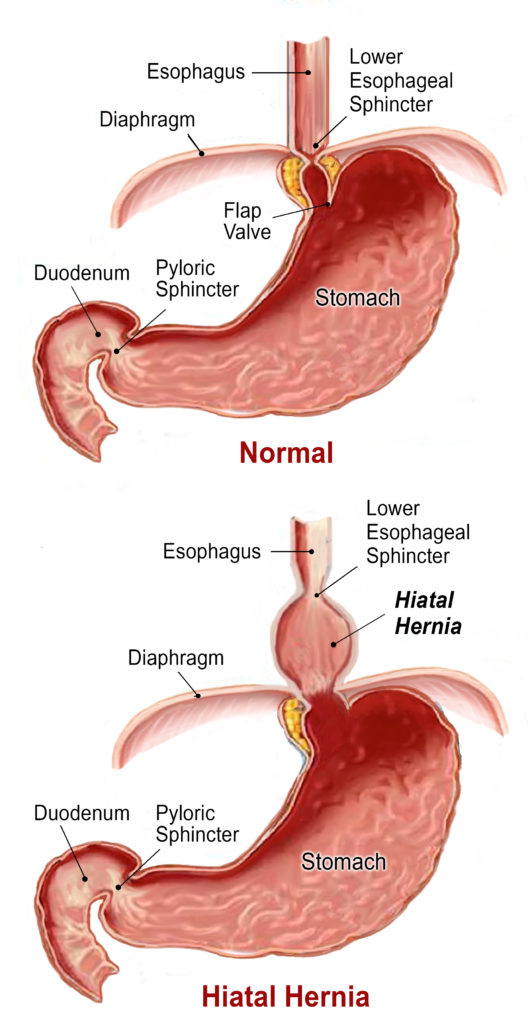
Unfortunately, the LES cannot close properly with a piece of the stomach wedged through the enlarged hiatal hole. As stomach acid refluxes back up into the esophagus, the person may experience heartburn, esophageal spasms, inflammation or sometimes ulcers. Hiatal hernia has been called the “great mimic” because it mimics many disorders. A person with gastroesophageal reflux disease, or GERD, may experience severe chest pains and think they’re in cardiac arrest, or stomachaches that feel like an ulcer. Due to the burning sensation many believe their stomach is producing too much hydrochloric acid and run for the “Tums.”
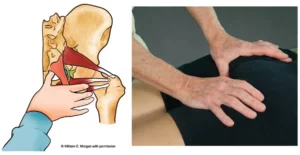
Poor posture may alter the position of the stomach, causing the hernia to squash the neighboring vagus nerve (Images 2a. & 2b.). Since this cranial nerve stimulates the release of hydrochloric acid (via proton pumps), this may cause over, or under, secretion of hydrochloric acid and stomach enzymes. It may also reflexively relax the pyloric sphincter at the bottom of the stomach, causing leakage of vital digestive juices. University of Michigan Medical School researchers found some cases where hiatal hernias were responsible for heart palpitations due to vagus nerve irritation.1
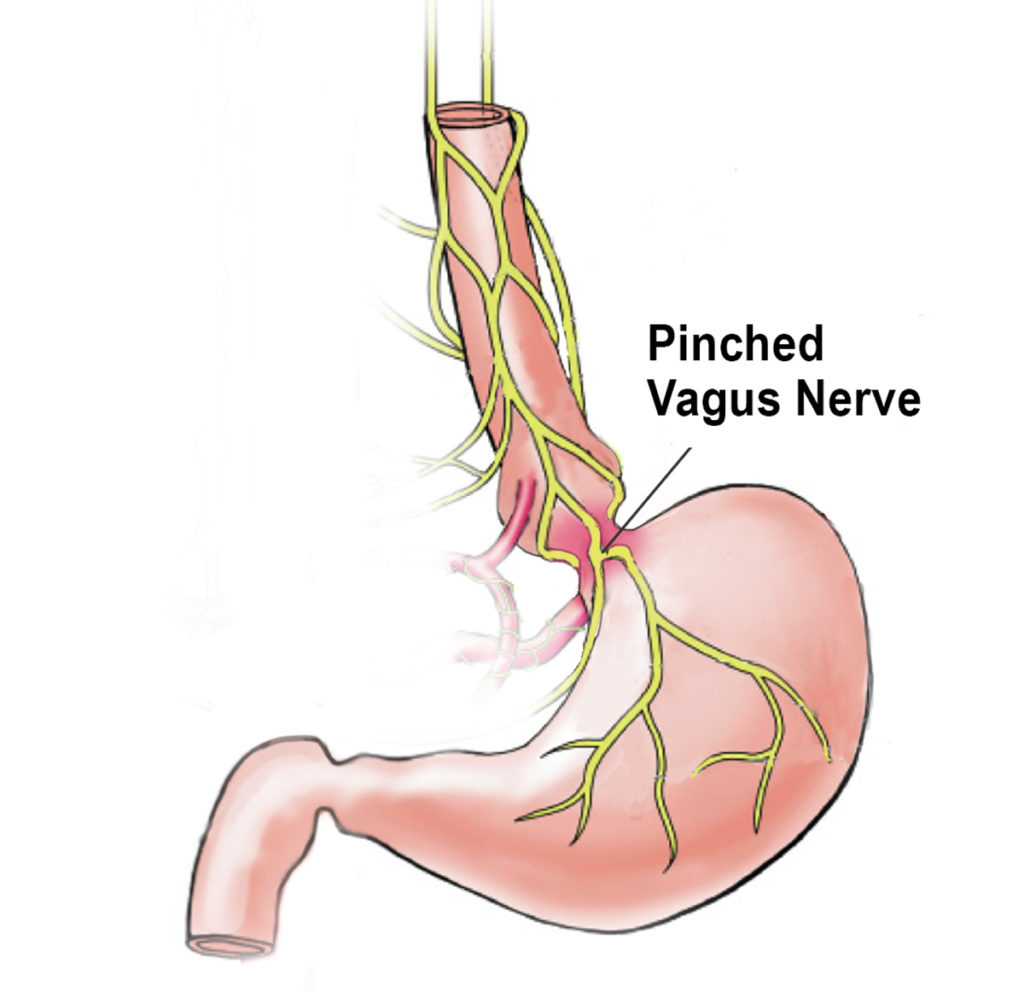
If a person develops poor stomach digestion due to a lack of hydrochloric acid, they will have difficulty digesting and assimilating protein and most minerals, causing food putrefaction in the intestines and accompanying whole-body toxicity. This lack of nutrition and toxic condition may contribute to food allergies, anemia, constipation, and immune and glandular system weaknesses. In chronic cases, gastric acid gas from food decay and fermentation causes throat spasms that lead to thyroid gland irritation and difficulty swallowing. Hiatal hernia sufferers often complain of not being able to “get pills and vitamins down….especially capsules”
The causes of a hiatal hernia are speculative and unique to each individual. However, there are a number of presumed possibilities. First of all there may be a mechanical cause. Hard coughing, sharp blows to the abdomen; tight clothing, obesity, and poor posture may contribute to the development of this problem. But, improper lifting may be the most damaging mechanical cause. If the air is not expelled from a person’s lungs while lifting, the intra-abdominal pressure may force the stomach through the diaphragm. When a person gets angry, they suck their breath upward and often fail to release the anger. In time, the abdominal fascia deforms and the stomach gets stuck up under the ribcage. I have observed that most clients presenting with severe hiatal hernias are dealing with extreme stress, sympathetic nervous system overload, and the inability to let go of all the anger and resentment.
The easiest way to assess for a hiatal hernia is to place your fingers on the upper belly just below the sternum. Take a deep inhalation and feel if your abs expand. If you lack anterior belly excursion and find yourself shoulder shrugging during deep inhalation, a hiatal hernia may be restricting diaphragmatic movement. Of course, there are many other, more complicated, methods of assessment, but this maneuver is fairly simple and reliable.
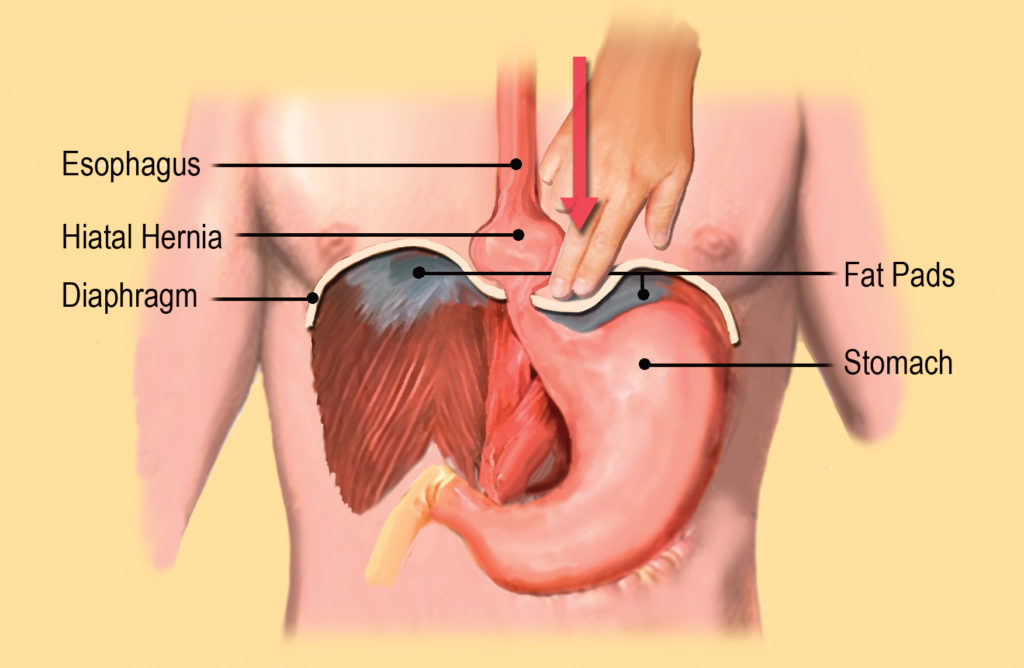
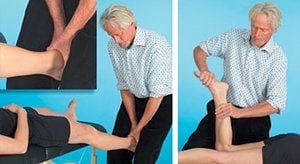
Since a hiatal hernia is primarily a mechanical problem, the easiest and best way to correct it is…mechanically (Image 3. ). Medical doctors attempt surgery to correct this disorder, but results tend to be poor. Cutting into this area can further weaken the diaphragm causing the hernia’s quick return. A better method is to manipulate the stomach and bring down the hernia by hand as demonstrated in the video below.
Note: Try timing how long your client can hold their breath before and after pulling the stomach down. It’s not unusual for chronic hiatal sufferers to be able to hold their breath a third longer after a good treatment. For optimum benefit, this hiatal routine must be done once a week until the person is symptom free. It’s also a good idea to teach clients how to do this simple procedure at home.
References
1. University of Michigan Medical School Clinical Cases: http://www.med.umich.edu/lrc/coursepages/m1/ anatomy2010/html/clinicalcases/hiatal_hernia/hiatal_hernia.html
On sale this week only!
Save 25% off the "Dalton Technique Treasures" eCourse
The “Dalton Technique Treasures” eLearning course is a compilation of some of Erik’s favorite Myoskeletal Alignment Techniques (MAT). Learn MAT techniques to assess and address specific sports injuries, structural misalignment, nervous system overload, and overuse conditions. ON SALE UNTIL April 29th! Get Lifetime Access: As in all our eLearning courses, you get easy access to the course online and there is no expiry date.