
Signs and Symptoms

Assess and Treat
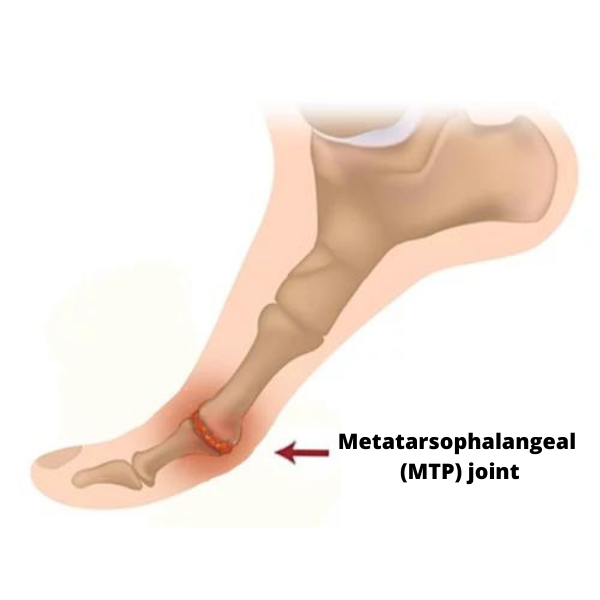
I’ve found the simple “Grind Test” very helpful in assessing for hallux limitus and rigidus. If the therapist is able to extend the client’s toe but pain or a crunchy noise is reported as the first MTP joint is compressed, hallux limitus may be suspected. Conversely, if pain or grinding is reported and the joint resists extension (even at mid-range), advanced hallux rigidus osteoarthritis could be the culprit.
Once I’ve identified a painful or immobile MTP joint, I begin to address it by performing graded exposure stretches to all lower leg, ankle, and foot musculature to increase flexibility and decrease reactive spasm. Next, I perform the following three Myoskeletal mobilization techniques:
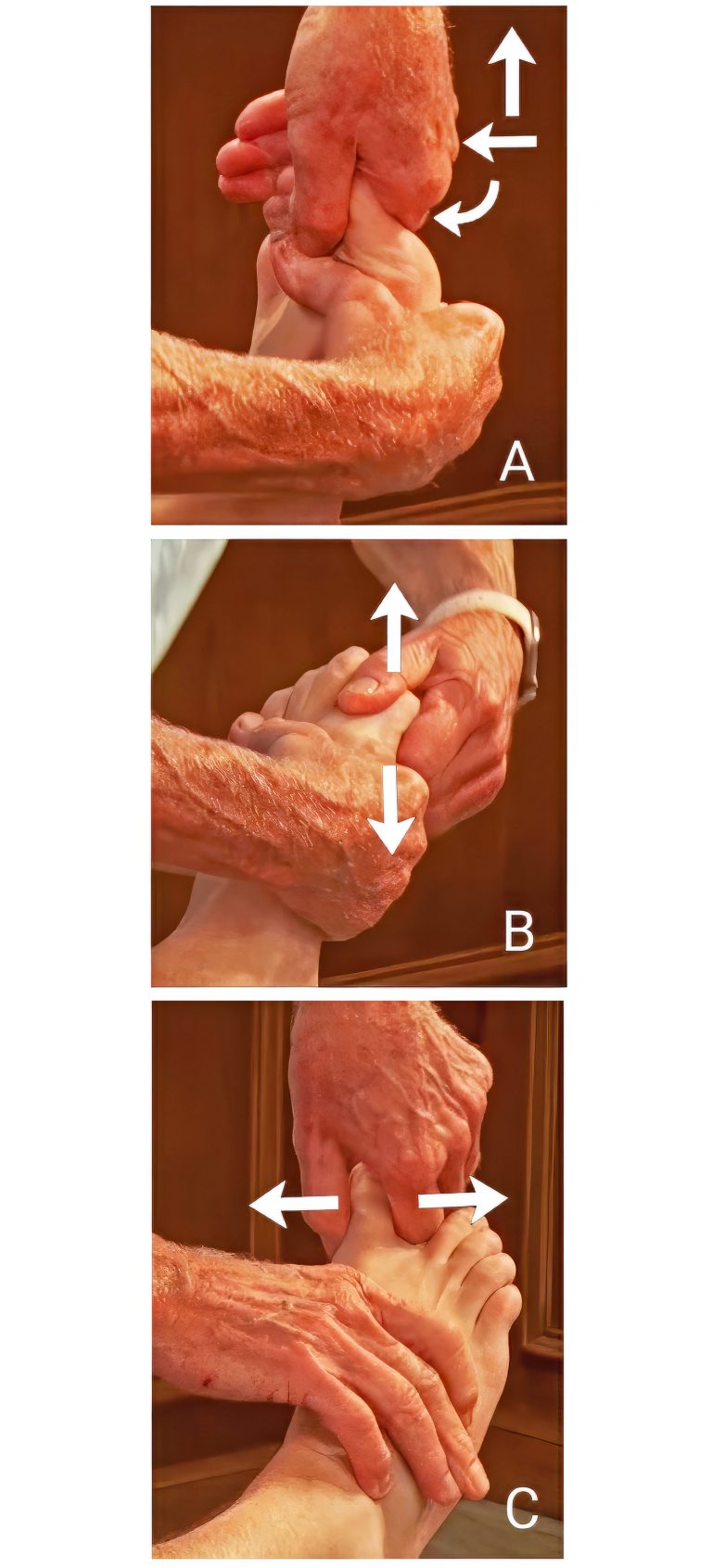
A. Long Axis Extension-Rotation: The therapist’s right hand braces the distal metatarsal bone while his finger and thumb slowly distract, extend, and rotate client’s proximal phalanx bone.
B. Dorsal and Plantar Glide: The therapist’s right hand braces the distal metatarsal bone while his finger and thumb glide the MTP joint up and down.
C. Abduction-Adduction: The therapist’s right hand braces the distal metatarsal bone while his finger and thumb abduct and adduct client’s proximal phalanx bone (joint translation).
Summary
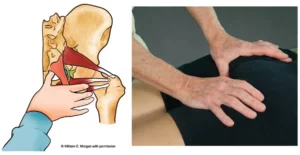
Limited first-toe extension leads to altered mobility at the talocrural joint. If the ankle can’t dorsiflex properly, the knee and hip will not fully extend. The result is decreased hip flexor flexibility and repeated extension-rotation of the lumbar spine. This is a prime example of how a kink in a lower extremity can affect structures further up the kinetic chain.
Myoskeletal Therapy employs low-force stretching maneuvers to reduce symptoms and improve MTP joint function. We’re encouraging the body to move rather than forcing it to do so, as forcing movement causes the brain to layer the area with protective muscle guarding. Along with manual treatments to improve MTP mobility, it’s essential to assign self-care exercises to help maintain the gains and further increase first-toe range of motion. Clients spend the majority of their time outside the clinic, so they must share responsibility for locking in the changes.
I’ve found clients are more likely to perform playful exercises, such as bouncing on a mini trampoline, hiking, and ankle rocking. The act of rocking in all directions with the feet dorsiflexed is one of the best and easiest ways to fully restore function of the feet, ankles, knees and hips synchronously — the way they’re designed to work. Give these assessment and treatment options a try in your own practice to help clients who present with stiff and painful hallux limitus and rigidus.
References
- Ho, B., & Baumhauer, J. (2017). Hallux rigidus. EFORT Open Rev, 2(1), 13-20.
- Greenman, P. (1992). Exercise as an adjunct to manual therapy, class notes. Michigan State College of Osteopathic Medicine.
On sale this week only!
Save 25% off the "Dalton Technique Treasures" eCourse
The “Dalton Technique Treasures” eLearning course is a compilation of some of Erik’s favorite Myoskeletal Alignment Techniques (MAT). Learn MAT techniques to assess and address specific sports injuries, structural misalignment, nervous system overload, and overuse conditions. ON SALE UNTIL April 29th! Get Lifetime Access: As in all our eLearning courses, you get easy access to the course online and there is no expiry date.