Assessing PMFR weakness as shown in the Assessment course
Addressing Postural Plasticity
Digital Dementia is a term coined by neuroscientist Manfred Spitzer to describe a condition caused by digital technology overuse that results in a breakdown of cognitive abilities. When most of us consider the term cognition we think of our ability to think, problem solve, or just do our work, but how many of us relate it to posture? Poor posture is not a cause as much as it is a symptom. Essentially, it is dysfunction of various systems in the body that are either over or under functioning. In most bodywork circles, we think of faulty posture as a ‘tissue issue’ and, in many cases problems do arise from strained or overused connective tissues and joints, but what about visual or balance (vestibular) disorders that may be compromising the brain’s sorting and switching stations?
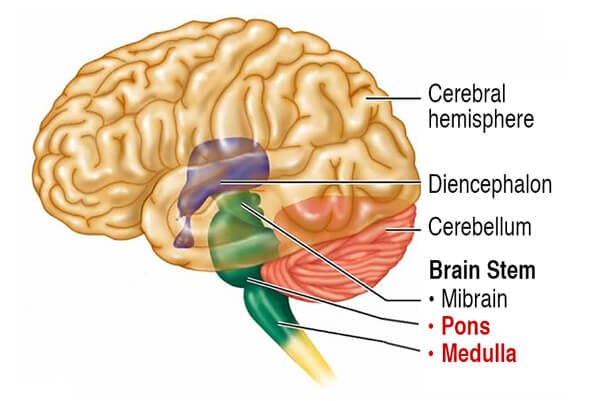
Ponto Medullary Reticular Formation (PMRF)
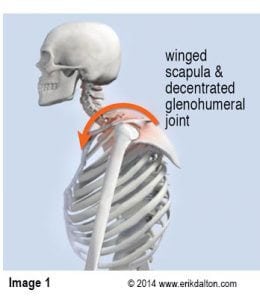
The PMRF is a dynamic relay station located in the brainstem at the pontomedullary junction where pons meets the medulla. It is considered the epicenter for postural control (Image 1.). The PMRF houses eight cranial nerves that carry out vital motor and sensory functions including eye-ear coordination that aids in head righting reflexes and balanced gait. When functioning properly, the PMRF inhibits cervicothoracic flexion, which, in turn, effectively resists gravitational exposure. Those clients with PMRF disorders may present with an Upper Cross Syndrome pattern, i.e., forward jutted chin, internally rotated arms, protracted shoulder girdle, and t-spine hyperkyphosis. Each day these bodies battle gravity and in the absence of experienced manual, movement and brain-based therapy, usually end up on the losing end.
Hours sitting staring at screens, lack of exercise, and poor body biomechanics all contribute to the symptom of poor posture, and may lead to other conditions such as lack of focus, visual disturbances, depression, poor balance, protective muscle guarding and more. When performing a postural assessment as part of a client’s intake exam, I’m not only looking at tissue issues, but more importantly, what the nervous system is doing with this information. For example, I may include proprioceptive challenges such as one-legged standing to assess for vestibular (balance) dysfunction, gaze stabilization exercises for visual disturbances or the Romberg (sway) Test for cerebellar weakness. Sensory impulses originating in the neck and ankles are particularly important. Proprioceptive input from the neck indicate the direction in which the head is turned and cues from the ankles indicate the body’s movement or sway relative to the ground.
As sensory integration takes place through good bodywork and corrective proprioceptive exercises, the brain stem transmits impulses to the muscles that control movements of the eyes, head and neck, trunk, and legs, thus allowing a person to both maintain balance and have clear vision while moving. Of course, there are multiple neurological systems that contribute to optimal posture. Our goal is synergistic integration of these systems to normalize and restore flexor/extensor synergy and postural stabilization during dynamic movement.
On sale this week only!
Save 25% off the Posture Pain Performance course!

NEW! USB version with enhanced video
Discover the foundational principles behind MAT technique as we take you on an in-depth look at the connection between pain, posture and function. Save 25% off the Posture Pain Performance course this week only. Offer expires Monday April 22nd. Click the button below for more information and to purchase the course. Upon completion receive 20CE hours and a certificate of completion to display in your office.
Bonus: Order the Home Study version and receive the e-Course for FREE!