What’s the cause of back pain?
Most of us suffer some form of neck and back pain during our lifetime. It’s just as common as a headache, stomachache or knee pain. “Until it was turned into a medical condition in the early 20thcentury, back pain was considered an inevitable human experience,” said Canadian surgeon Hamilton Hall, MD. “There is no simple cure because there is usually not a clear-cut precipitating trigger associated with many forms of musculoskeletal pain,” notes Hall.
Despite the liberal use of the words “back injury” across modern societies, most episodes of back pain do not have an obvious cause. “Research indicates that approximately two of every three people who experience pain in the spine are unable to identify any specific event that may have caused their problems,” states Hall. Back pain simply happens!
The modern perspective that neck and back pain is a variable, intermittent illness rather than a one-time condition should not be considered a threatening event for our clients. In the vast majority of cases, recurrences of these painful conditions are not signs of advancing disease, an omen of chronic disability or even a cause for significant worry.
Some researchers draw an analogy between back pain and upper respiratory infections. Many individuals contract colds or respiratory infections several times each year, yet are typically not viewed as a significant threat to their health. Colds don’t
require high-tech diagnostic testing, heroic treatment interventions or significant absence from work. These conditions, like most cases of neck/back pain, simply are bumps in the road.
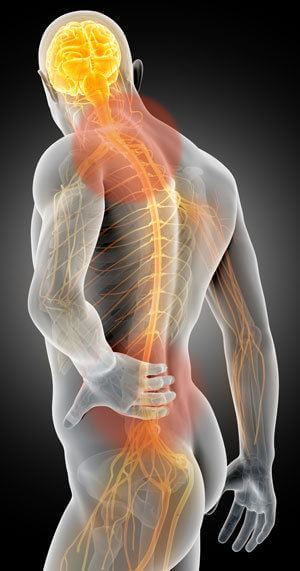
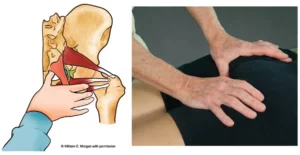
Traditional massage techniques are helpful in desensitizing hyperexcited cutaneous (skin and fascial) neuroreceptors. However, deep-tissue techniques that incorporate active client movements (enhancers) during the hands-on work, add additional therapeutic power by calming articular (joint) receptors and improving proprioception and body awareness.
Intrinsic muscles and joints are inseparable; what affects one always affects the other. Therefore, myofascial pain syndromes should include soft-tissue techniques that create extensibility in contractured tissues via graded exposure (repeated non-painful movements), tonify weak muscles, and decompress impacted, motion-restricted joints and their supporting ligaments.
As the research rolls in and causality is eventually decided, it is in the client’s best interest to immediately begin routinely scheduled bodywork sessions in conjunction with a specialized corrective exercise regime… regardless of origin. Well structured manual therapy sessions and individualized rehabilitation programs appear to be the treatment of choice for this chronic and sometimes disabling condition that affects an estimated 2 million Americans each year.
On sale this week only!
Save 25% off the "Dalton Technique Treasures" eCourse
The “Dalton Technique Treasures” eLearning course is a compilation of some of Erik’s favorite Myoskeletal Alignment Techniques (MAT). Learn MAT techniques to assess and address specific sports injuries, structural misalignment, nervous system overload, and overuse conditions. ON SALE UNTIL April 29th! Get Lifetime Access: As in all our eLearning courses, you get easy access to the course online and there is no expiry date.