Treating Suboccipitals and Dural Drag
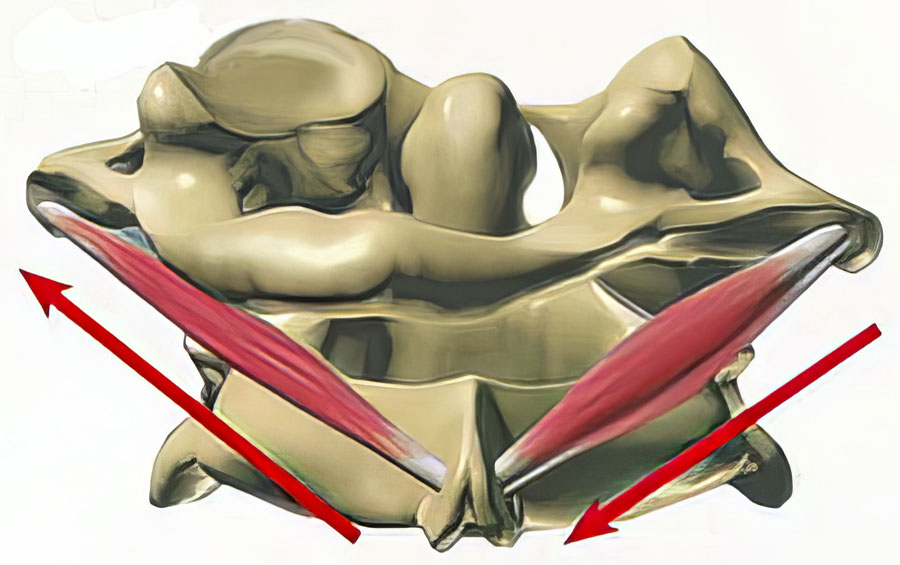
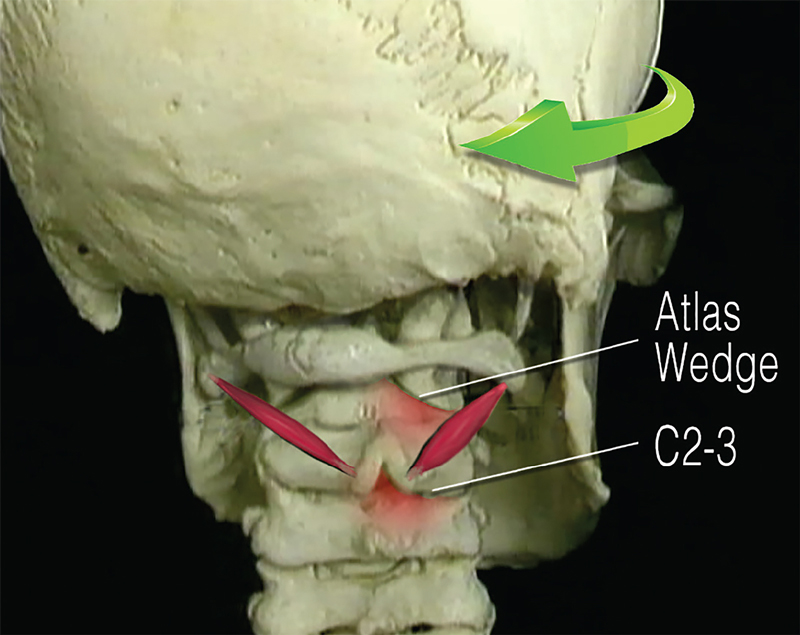
The obliquus capitis inferior (OCI) muscles may be the most underappreciated of all the suboccipitals. Arising from the spinous process of C2 (axis) and inserting on the transverse process of C1 (atlas), their primary function is head-on-neck rotation. Notice in Image 1. how the overstretched left OCI creates reciprocal shortening on the right.
During intake exams, habitual stomach sleepers often recount waking one morning unable to turn the head left without triggering upper neck and head pain. Many of these stomach-sleeping headaches are rooted in neurovascular tension or compression from mechanical strain. In this article, I’ll present cervicogenic headache research, propose biomechanical explanations, and demonstrate Myoskeletal Alignment Techniques (MAT) for treating stomach-sleepers’ headaches.
Mechanoreceptive and nociceptive bombardment from overstretched spinal ligaments, joint capsules, and suboccipital muscles may wreak enough havoc to convince the brain to protectively guard or elicit pain. Image 4, 5 and 6 demonstrate an effective MAT routine for releasing hypercontracted right-side OCI muscles, a gentle atlas-axis alignment technique, and a graded exposure stretch to relieve sympathetic guarding. Since the nervous system directs all bodily functions, it behooves today’s therapist to acquire skills for treating mechano-sensitivity in neural structures. Some therapists engage the nervous system via gentle skin manipulation, some through fascial stretch, and others, such as myself, include mobilizations for bones attaching to the dura mater.
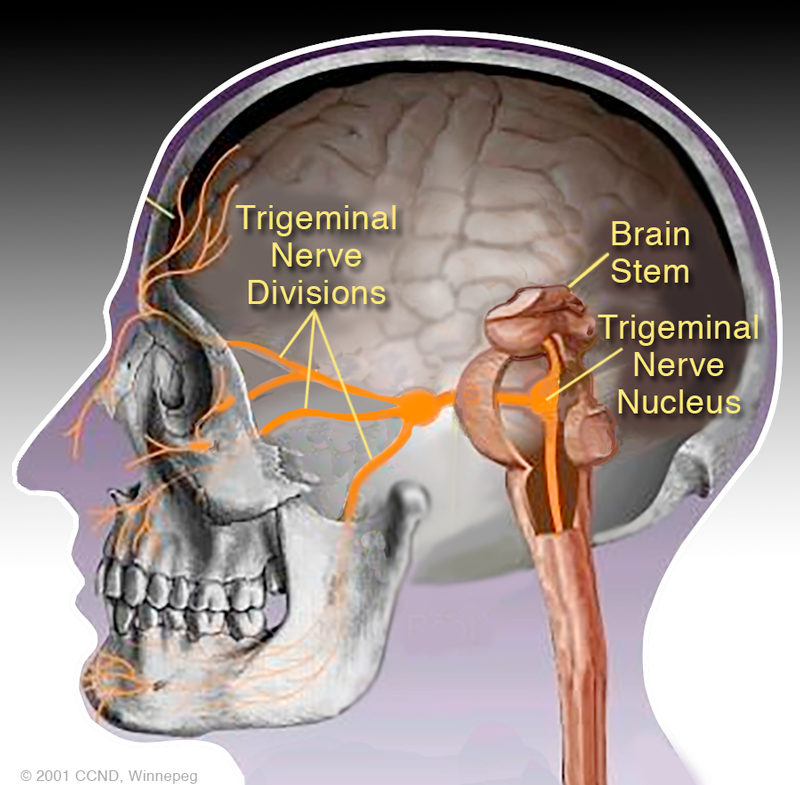
Biomechanical Explanations
MAT Routine:
Releasing Hypercontracted Right-side OCI Muscles
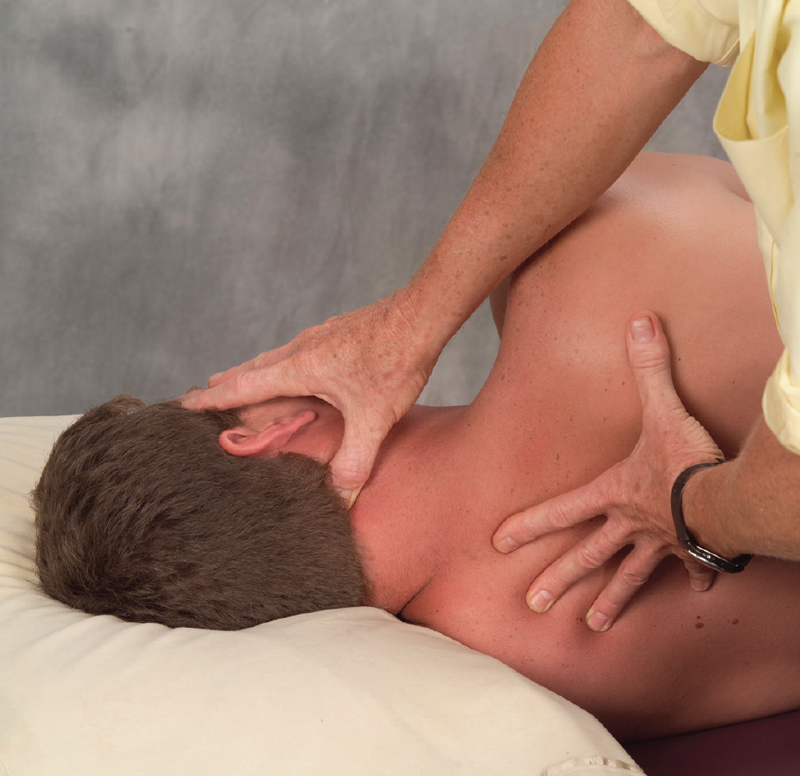
- The therapist’s hands drape the client’s head and their right thumb contacts the C2 spinous process and glides slightly superolaterally on the inferior oblique muscle.
- The client inhales while gently right rotating their head against the thumb and hand resistance.
- As the client exhales, the therapist’s thumb maintains sustained inferior oblique pressure as the client slowly left rotates the head.
- Repeat 3 to 5 times and retest.
Gentle Atlas-Axis Alignment Technique

- With elbows on the table, the therapist flexes the client’s head 45 degrees and right rotates to the first restrictive barrier.
- The client gently left rotates against the therapist’s resistance to a count of five, rests, and therapist right rotates to the new restrictive barrier.
- Repeat with rotation to the left side.
Graded Exposure Stretch To Relieve Sympathetic Guarding
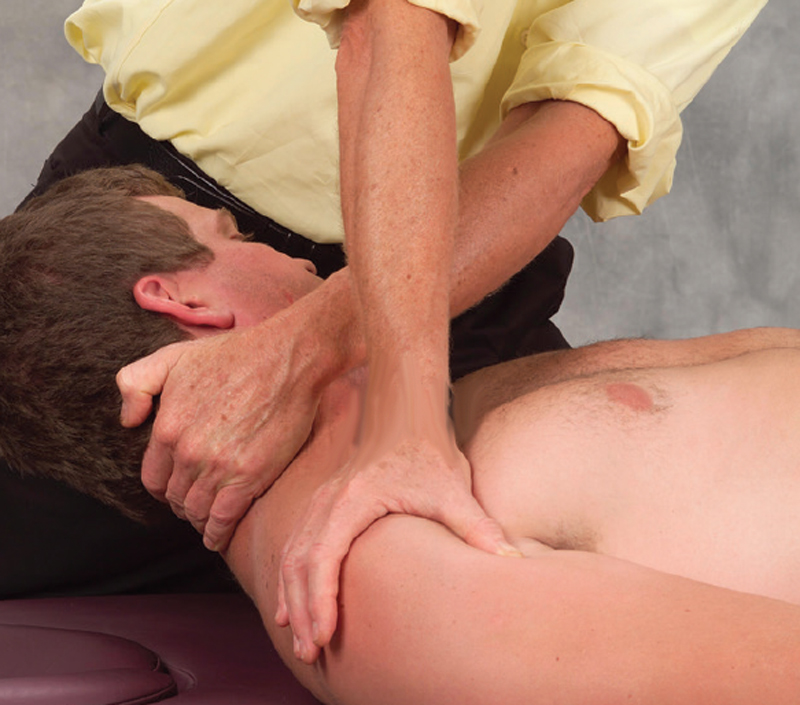
- Keeping the client’s head flexed at 45 degrees, the therapist uses a counterforce to slowly rotate and drag the neck fascia superiorly.
- Repeat.
Clients must understand that the brain is their best friend, and pain is there to protect their body from further perceived insult. It’s tempting but counterproductive to tell clients their pain results from muscle spasm, trigger points, or bones out of place. Clients simply need to be reassured they are in a safe place, and that everything is all right, right now.
References
- N. Bogduk, “Anatomy and Physiology of Headache,” Biomedicine & Pharmacotherapy 49, no. 10 (1995): 435–45
- F. Scali, E. S. Marsili, and M. E. Pontell, “Anatomical Connection Between the Rectus Capitis Posterior Major and the Dura Mater,” Spine 36, no. 25 (December 2011): E1612–4.
On sale this week only!
Save 25% off the Posture Pain Performance course!

NEW! USB version with enhanced video
Discover the foundational principles behind MAT technique as we take you on an in-depth look at the connection between pain, posture and function. Save 25% off the Posture Pain Performance course this week only. Offer expires Monday April 22nd. Click the button below for more information and to purchase the course. Upon completion receive 20CE hours and a certificate of completion to display in your office.
Bonus: Order the Home Study version and receive the e-Course for FREE!